When Depression Doesn't Respond to Other Treatments
For teenagers and adolescents who are still struggling despite therapy and medication, TMS offers a safe, non-invasive path forward. It is FDA-cleared, requires no anesthesia, and fits around school and everyday life.
Non-Invasive
No surgery, no sedation
TMS uses focused magnetic pulses to stimulate specific areas of the brain. There is no anesthesia, no hospitalization, and no recovery time — your teen is awake and alert throughout each session.
Minimal Side Effects
Well tolerated by adolescents
Unlike antidepressants, TMS does not cause weight gain, sexual side effects, or sedation. Most teens tolerate it very well, and any early discomfort typically resolves within the first few sessions.
Life Goes On
No disruption to school or activities
Sessions are outpatient and typically 20–40 minutes long. Your teen can drive or be dropped off, and return to school or other activities immediately after each appointment.
What Is TMS Therapy?
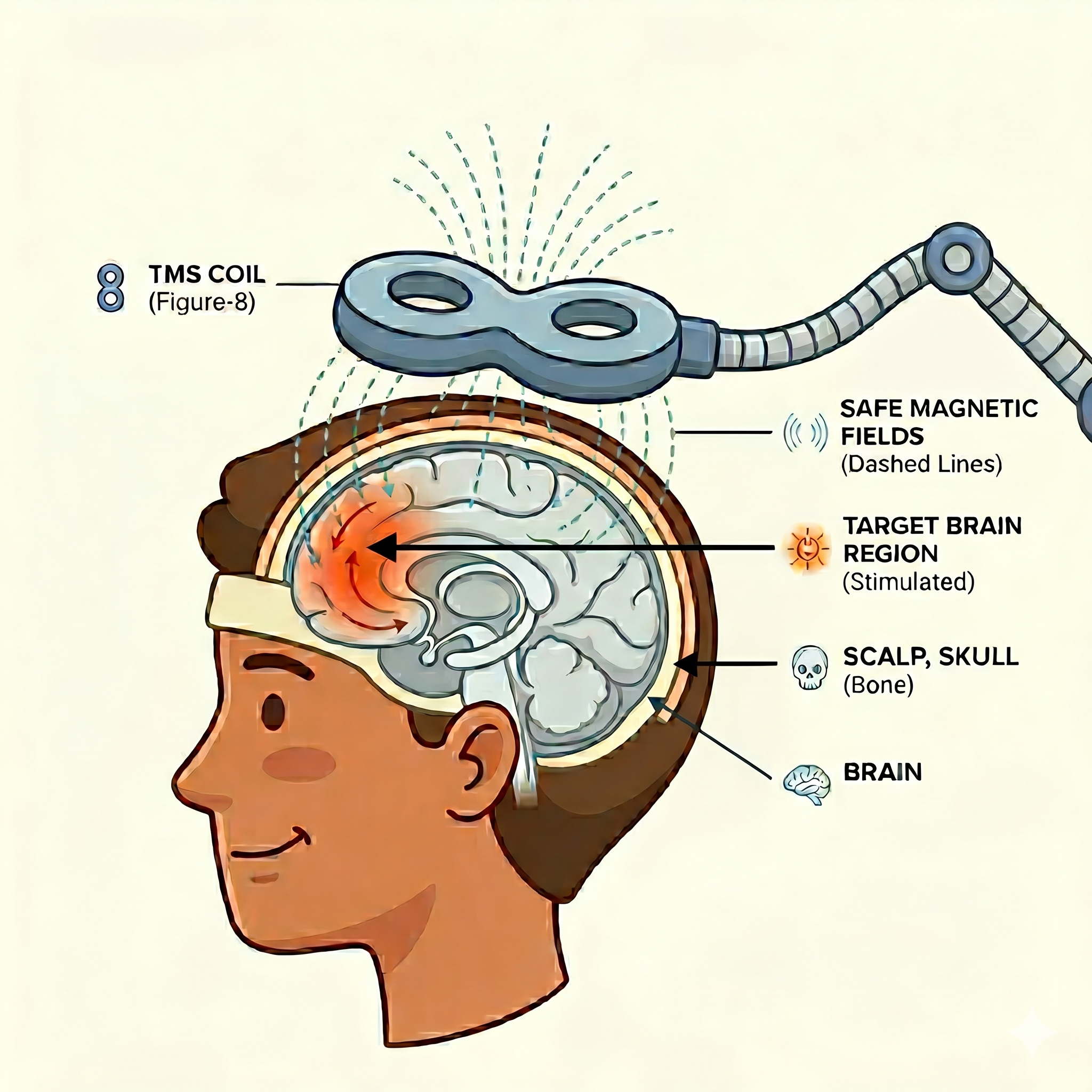
Transcranial Magnetic Stimulation (TMS) uses brief, focused magnetic pulses — similar in strength to those used in an MRI — to stimulate nerve cells in the part of the brain involved in mood regulation. It is a well-established treatment for depression in adults and an emerging option for adolescents.
No Anesthesia Required
Your teen stays fully awake during treatment — there is nothing to recover from afterward.
Outpatient Treatment
Sessions take place at our Menlo Park clinic. Your teen can listen to music, watch a show, or scroll on their phone during the session.
Immediate Return to Normal Activity
After each session, your teen can go straight to school, sports practice, or any other activity with no restrictions.
Types of TMS for Adolescents
There are two main TMS protocols used for teens and adolescents. The right approach depends on your teen's clinical picture, schedule, and family goals — something we evaluate carefully before recommending any plan.
Standard TMS
Longer, conventional protocol — compacted daily adjunctive treatment over several weeks
Standard TMS is the most established protocol for adolescents. It is typically used alongside (adjunctive to) ongoing therapy or medication, rather than as a standalone replacement. A standard course consists of daily sessions, five days per week, for six to nine weeks — approximately 30 to 36 sessions in total. Each session lasts 20 to 40 minutes.
Standard TMS is generally considered for adolescents aged 15 and older who have not achieved adequate improvement with at least one antidepressant trial or course of psychotherapy. It is supported by a growing body of clinical research in adolescent populations.
Accelerated TMS — SAINT / SNT Protocol
Shorter, intensive protocol — all-day treatment over 5 days, one-day options emerging for teens
Accelerated TMS delivers multiple TMS sessions per day over a compressed timeframe — typically five days — rather than spreading treatment over several weeks. The Stanford Accelerated Intelligent Neuromodulation Therapy (SAINT), also known as Stanford Neuromodulation Therapy (SNT), is one such protocol that has shown rapid antidepressant effects in adults.
Research into accelerated and one-day TMS protocols for adolescents is an actively developing area. While these approaches are not yet standard of care for teens, they represent a promising frontier — particularly for situations where a faster response is important or where a condensed treatment schedule is preferred. We evaluate each adolescent individually to determine whether an accelerated approach is appropriate and evidence-supported for their situation.
What Does a TMS Session Feel Like?
Many teens and their families want to know what to expect before the first session. Here is an honest, practical description.
A Tapping or Knocking Sensation
Most patients describe TMS as a rhythmic tapping or knocking feeling on the scalp over the treatment area. It is not described as painful by most people — more of an unusual but tolerable sensation.
Mild Discomfort in Early Sessions
Some teens experience mild scalp discomfort or a headache during or after the first few sessions. This is normal and typically fades as the brain and scalp adjust to the stimulation over the first week.
Adjustments Are Easy
We can adjust the intensity and positioning of the coil to improve comfort at any time during sessions. Your teen's feedback is important to us, and we work to ensure each session is as comfortable as possible from the start.
Something to Do During the Session
Your teen can use headphones, watch something, text friends, or just relax in the chair. The session runs in the background while they do whatever feels comfortable.

Is TMS Safe for Teenagers?
Safety is the first question every parent asks — and it is the right one. Here is what the evidence and our clinical experience show.
Well Tolerated
Clinical studies in adolescents consistently show that TMS is well tolerated, with low dropout rates due to side effects. Most teens complete their full course of treatment.
Temporary, Localized Side Effects
The most common side effects are temporary scalp discomfort and headache, both of which are localized and typically resolve on their own within the first week of treatment.
Physician Oversight Throughout
TMS in adolescents requires careful clinical oversight. Our board-certified child and adolescent psychiatrist conducts a thorough evaluation before treatment begins and monitors progress throughout the course — this is not a set-it-and-forget-it approach.
No Risk of Dependence
TMS is not habit-forming and carries no risk of dependence or withdrawal — a meaningful advantage when treating adolescents during formative years.
Growing Evidence Base
Research on TMS in adolescents is a rapidly growing area. While the evidence base is still developing compared to adults, multiple clinical trials have demonstrated meaningful antidepressant effects with a favorable safety profile.
Who May Be a Good Candidate?
TMS is not the first step — it is for teens who have already tried other approaches and are still struggling. The following situations are common starting points for a conversation about TMS.
Still Depressed Despite Treatment
Persistent symptoms despite effort
Your teen has engaged in therapy, tried medication, or both — and their depression has not lifted to a meaningful degree. TMS offers a different mechanism of action that may succeed where other approaches have not.
Inadequate Response to Therapy or Medication
Partial or no improvement
Some teens respond partially to antidepressants or psychotherapy but never achieve full remission. TMS can be used adjunctively — alongside existing treatments — to help bridge that gap.
Difficulty Tolerating Medication
Side effects that interfere with daily life
Weight changes, emotional blunting, sleep disruption, and other medication side effects can be especially disruptive during adolescence. TMS provides an effective option with a very different side effect profile.
Family Interest in a Non-Medication Option
Preference for non-pharmacological treatment
Some families prefer to minimize or avoid psychiatric medications for their teenager. TMS offers a clinically meaningful, evidence-informed alternative for adolescents with moderate-to-severe depression.
Prior Hospitalization or Intensive Treatment
History of more acute care
Teens with a history of psychiatric hospitalization, partial hospitalization, or intensive outpatient programs who remain symptomatic in outpatient care may benefit from TMS as a next step in their treatment.
School and Life Impairment
Depression affecting functioning
When depression is significantly affecting school attendance, grades, relationships, or activities, TMS may offer a more impactful intervention than continued medication adjustments alone.
Individualized, Evidence-Informed Care
TMS in adolescents is not a one-size-fits-all intervention. Every teenager who comes to Palo Alto TMS undergoes a thorough psychiatric evaluation before any treatment recommendation is made. We consider the full clinical picture — the evidence, the family's priorities, and the practical realities of school and life — before recommending a course of action.
Psychiatric Evaluation First
Before any TMS begins, we conduct a comprehensive psychiatric evaluation to confirm diagnosis, review treatment history, and assess whether TMS is the right next step for your teen.
Stanford-Trained, Board-Certified Child Psychiatrist
Our physician is a board-certified child and adolescent psychiatrist with Stanford training and nearly 20 years of clinical experience. Adolescent neurodevelopment and psychiatric care is our area of deep expertise.
Family-Centered Decision-Making
Families are active partners in the treatment process. We take time to explain the evidence, answer questions honestly, and incorporate family preferences alongside clinical recommendations.
Scheduling Around School & Life
We work with families to build a treatment schedule that minimizes disruption to school, extracurriculars, and other commitments. Treatment should support recovery — not create new obstacles.

Insurance Coverage for Teen TMS
TMS therapy is often covered by insurance — including for adolescent patients. Prior authorization is usually required, and our team handles that process on your behalf.
Often Covered
For treatment-resistant depression
Many major insurance plans cover TMS for adolescent patients with treatment-resistant depression, particularly when prior medication or therapy trials have been documented. We are in-network with Aetna, Anthem, Blue Shield of California, Carelon, Cigna, Evernorth, Magellan, and Optum.
Prior Authorization Required
We manage it for you
Most insurers require prior authorization before TMS treatment begins. Our clinical team prepares and submits all required documentation — treatment history, clinical records, and a letter of medical necessity — and follows up with your insurer until approval is secured.
Benefit Verification at No Charge
Know your costs before you commit
We verify your teen's insurance benefits before treatment begins and walk you through any expected out-of-pocket costs — so there are no surprises. This service is provided at no charge.
Ready to Learn More?
If you are a parent or guardian exploring TMS for your teenager, we encourage you to reach out. We are happy to answer your questions, discuss your teen's situation, and help you decide whether an evaluation makes sense — with no obligation.
Patient & Family Resource
TMS for Teens — Information Handout
Download our one-page overview of TMS therapy for teenagers and adolescents — useful for sharing with your teen, a referring provider, or school counselor.
Download PDF Handout